What is it?
The shoulder joint has one of the most flexible range of movement out of all the joints in the body. This flexibility comes at the expense of stability (keeping the ball in the socket). The shoulder is at it’s most vulnerable and unstable position when it is overhead and extended backwards such as contact to the arm when catching a ball overhead.
The shoulder joint can dislocate with the ball moving off the front or the back of the socket. The most common direction of a traumatic dislocation is off the front or anterior dislocation.
Dislocations often lead to a painful clunk and deformity in the shoulder. The dislocated parts can sometimes go back into position spontaneously or require manipulation to reposition the joint.
What injuries occur in a shoulder dislocation?
Injuries can tear many of the supporting structures around the shoulder. These include:
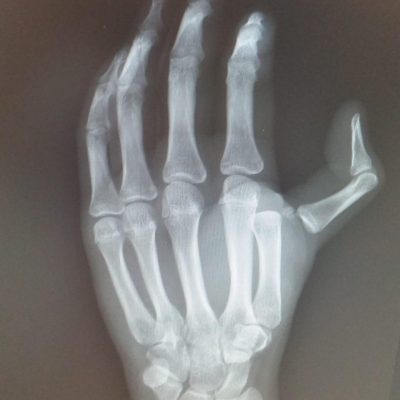
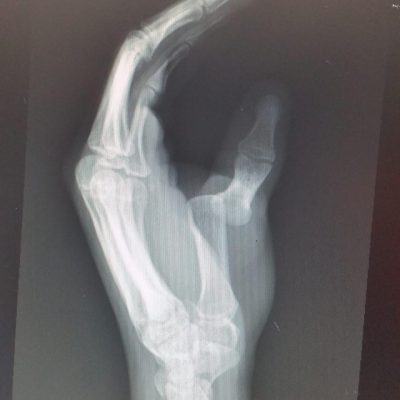
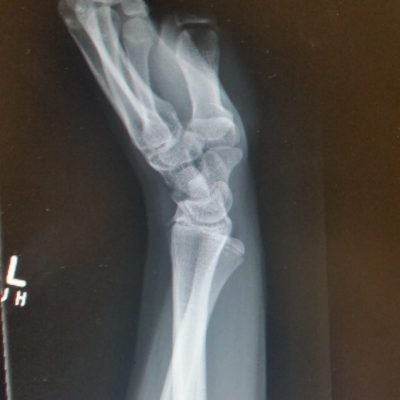
Bone – Fractures or impaction injuries can occur as the ball falls out of the socket. A bony Bankart injury is a fracture of the front edge of the socket (anterior glenoid fracture). A Hill-sachs lesion is an indentation fracture in the back of the ball or humeral head.
Labrum – This is the supporting rim of cartilage around the socket or glenoid. It is often torn at the from and bottom of the socket in an anterior dislocation. This is termed a Bankart lesion and is often the cause of ongoing instability in younger patients.
Capsule and ligaments – These are the soft tissues that act as a sack that covers the ball and socket. They can be stretched or torn during a dislocation.
Rotator cuff – This is a group of 4 muscles and tendons that attach to the top of the ball of the shoulder. They are responsible for controlling movements off the shoulder. If there is persistent pain and weakness in the shoulder beyond 3 weeks this can be a sign that the rotator cuff tear has been torn at the time of dislocation and warrants further scans and possible surgery.
Nerves – When the shoulder dislocates, it can stretch the nerves that pass in front of the shoulder and lead to persistent weakness. Fortunately, in most situations, these nerves recover but can take over a year, especially in older patients.
What is the treatment?
Treatment for shoulder dislocations depends on the age of the patient, activity level, shoulder examination and injured structures.
Younger patients who want to return to contact sport or overhead throwing will often require surgery to prevent repeated episodes of dislocation or subluxation (partial dislocation).
Older and less active patients can do well with physiotherapy to help strengthen the other supporting structures around the shoulder which is often successful in preventing further instability.
What to expect with surgery?
Shoulder stabilisation surgery or shoulder reconstruction commonly refers to repair of the torn labrum to the front of the socket. This is commonly done using 2 or 3 1cm cuts around the shoulder using arthroscopic or keyhole surgical techniques. Patients are admitted into hospital, usually overnight but can also be performed as day surgery. Physiotherapy is an important component of successful rehabilitation to regain flexibility and strength whilst protecting the repair. A sling is usually required to be worn for 3-6 weeks.
As a guide, you should expect the following timeframes for return to activity:
Driving: 6-8 weeks
Office work: 2-3 weeks
Manual work: 12 weeks
Contact sport: 3-6months